Transplantation of a “lower-quality” kidney to a person in end-stage renal failure is more cost-effective and has greater quality-of-life benefit than remaining on dialysis waiting for a better kidney, a health economics study has found.
- Health economics study helps solve marginal quality kidney transplant vs dialysis dilemma
- Donor kidneys in demand around the world
- Transplanting a kidney of any quality is cost-effective and better strategy than remaining on dialysis
Health economist at Australian Centre for Health Services Innovation (AusHSI), Dr Sameera Senanayake said health systems around the world had been unable to meet growing demand for kidney transplants.
He said around 100,000 kidneys were transplanted globally in any year while more than 100,000 patients in the US alone were waiting for a kidney.
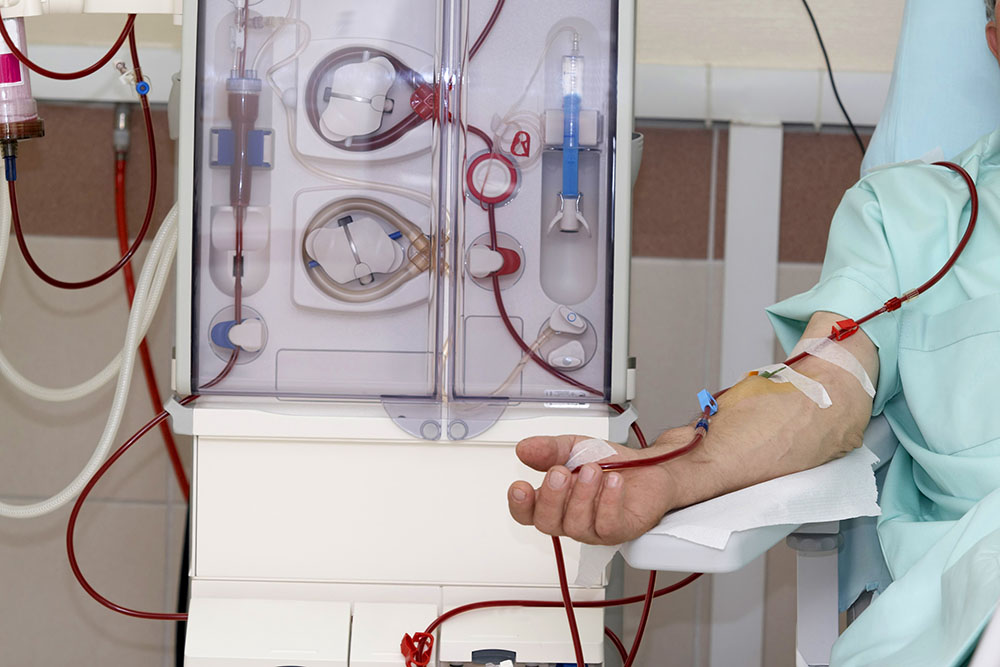
People with end-stage renal failure need dialysis three times a week, an onerous process for patients and an expensive treatment. Mortality is higher for dialysis patients than for those with successful transplants.
Dr Senanayake said only 25 per cent of people on dialysis were on the waitlist for a deceased donor kidney transplant.
“Haemodialysis is associated with poor quality of life and mortality compared to transplantation,” Dr Senanayake said.
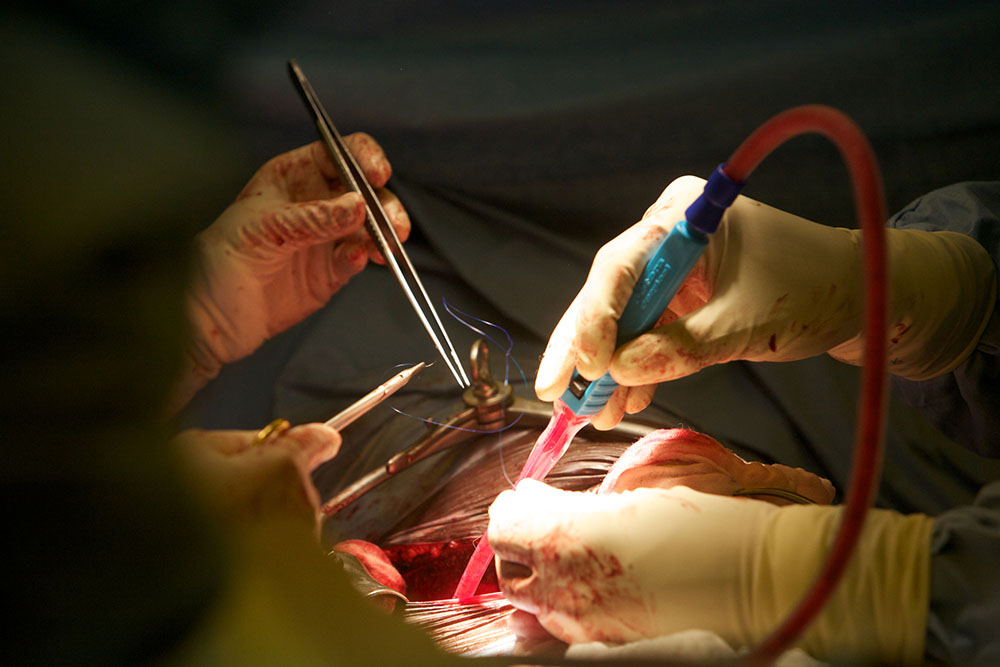
“It is common knowledge among the kidney community that if there were no shortage of donor kidneys, most of the patients on dialysis would be waitlisted and would ultimately receive a kidney.
“Compared to available renal replacement therapies, renal transplantation has dramatically improved the quality of life and the mortality rate of patients with end-stage renal disease.
“Deceased donor kidneys are graded for quality according to criteria which include age, history of hypertension or diabetes and cause of death.”
Dr Senanayake said the shortage of donor kidneys and the high demand for them had led to the suitability criteria for deceased donor kidneys being expanded and more marginal-quality kidneys being used.
“However, low and marginal-quality kidneys have tended to be discarded due to the greater likelihood of higher risk of graft failure, delayed graft function and increased medication costs for the health service,” he said.

“Patients and doctors are faced with a dilemma ‘do I accept a kidney that may not be the best or do I wait for a better kidney?’”.
Dr Senanayake’s study is the first economic evaluation to assess the cost-effectiveness of transplanting deceased donor kidneys of different qualities.
“It is the first to assist patients and clinicians in making decisions on accepting a marginal quality kidney or remaining on dialysis while waiting for a better-quality kidney,” he said.
“The average age of kidney transplant in Australia is 51 years. This study analysed three age groups – 40, 50 and 60 years - from the Australia and New Zealand Dialysis and Transplant Registry which reports outcomes of dialysis treatment and kidney transplantation for end-stage kidney disease patients.
“We modelled different treatment scenarios and outcomes, including quality of life improvements, and four grades of donor kidneys against each age group.
“We found that transplanting a kidney of any quality is cost-effective and more beneficial in terms of quality of life for patients compared to remaining on dialysis.
“We found it is not a cost-effective strategy for any age group to depend on dialysis in hope of receiving a higher quality kidney.”
Dr Senanayake said the study could nudge health providers to reduce the discard rates of low-quality kidneys in favour of more kidney transplants and seek funding to remove the short-term financial disincentives inherent in transplanting low-quality kidneys.
Donor kidney quality and transplant outcome: An economic evaluation of contemporary practice was published in Value in Health.
QUT Media contacts:
Niki Widdowson, 07 3138 2999 or n.widdowson@qut.edu.au.
After hours: Rose Trapnell, 0407 585 901 or media@qut.edu.au.

