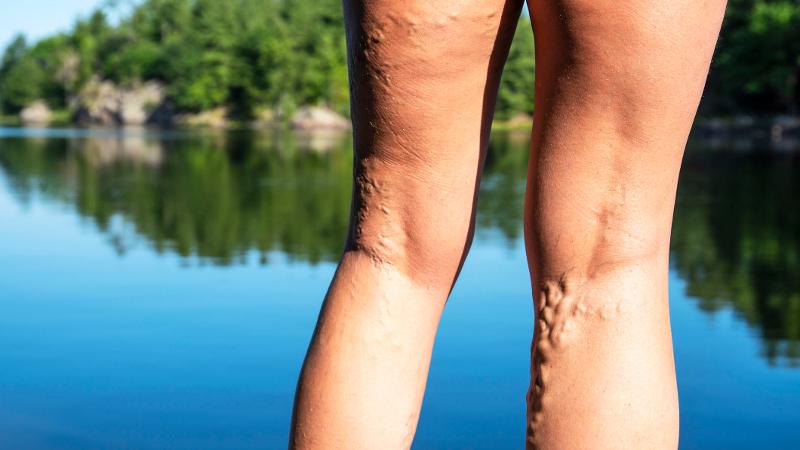
Some 500,000 Australians live with the daily burden of a wound that does not heal, but a risk assessment tool that provides an ‘early warning’ of which venous leg ulcer wounds need specialised treatment has been developed by QUT’s Dr Christina Parker.
- Half a million Australians are living with chronic wounds
- A new risk assessment tool can indicate wounds that require extra early intervention
- 25 per cent of people with chronic venous leg ulcer wounds are under 65
- People in jobs where a lot of standing is required are susceptible to venous leg ulcers
Dr Parker’s presentation on the assessment tool and its potential to help curb the $4 billion annual cost of treating chronic wounds received the top award at the CRC Association Collaborate Innovate 2019 Conference last week.
“The tool is simple,” Dr Parker, from QUT’s Institute of Health and Biomedical Innovation, said.
“It collects variables, such as the patient’s age, the area of the wound, whether high compression stockings or bandages are used, to predict with 80 per cent accuracy which wounds need early extra intervention or a referral to a specialist.
“This early intervention guides appropriate wound management and saves time and resources, and can reduce patients’ pain, distress and lifestyle limitations.”
Dr Parker’s presentation focussed on a case study of a woman who had endured a venous leg ulcer for 15 years, but, she says, further research has focussed on all types of wounds such as diabetic foot ulcers which are also hard to heal.
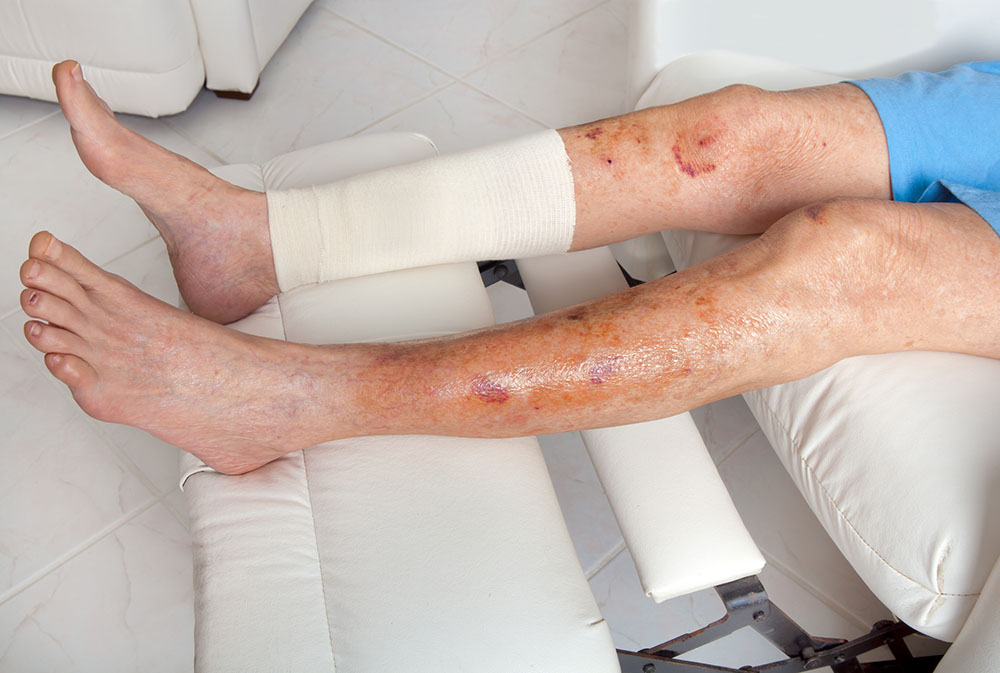
“Until you’ve had one, most people don’t realise the financial and social cost to the patient from wounds that do not heal,” she said.
“The woman in my case study had had a chronic wound for more than 15 years, not the same wound but she had never been without a wound in all that time.
“She had even been asked to leave a coffee shop owing to the amount of ooze and smell coming from her wound.
“Consequently she no longer meets friends at coffee shops and has sometimes been unable to pay to attend senior citizens’ outings due to the costs of dressings, appointments and medications.”
Dr Parker said venous ulcers made up 70 per cent of all leg ulcers.

“Veins can be damaged as we age but 25 per cent of people with chronic wounds are under 65 and this has a significant impact on their ability to work and quality of life. People who spend a lot of time on their feet such as nurses and hairdressers can be prone to venous leg ulcers.”
The risk assessment tool has already been developed into a computer and mobile application. Dr Parker is leading validation of the tool in the UK, Vienna and New Zealand, and it has been used to guide research in Canada.
Dr Parker was interviewed by ABC Canberra on her research.
Dr Parker’s research on validating the tool was published in the International Wound Journal.
The development of the tool was discussed in this validation:
Parker, Christina N., Finlayson, Kathleen J., & Edwards, Helen E. (2017) Predicting the likelihood of delayed venous leg ulcer healing and recurrence: Development and reliability testing of risk assessment tools. Ostomy Wound Management, 63(10), pp. 16-33.
QUT Media contacts:
Niki Widdowson, 07 3138 2999 or n.widdowson@qut.edu.au
After hours: Rose Trapnell, 0407 585 901 or media@qut.edu.au.


