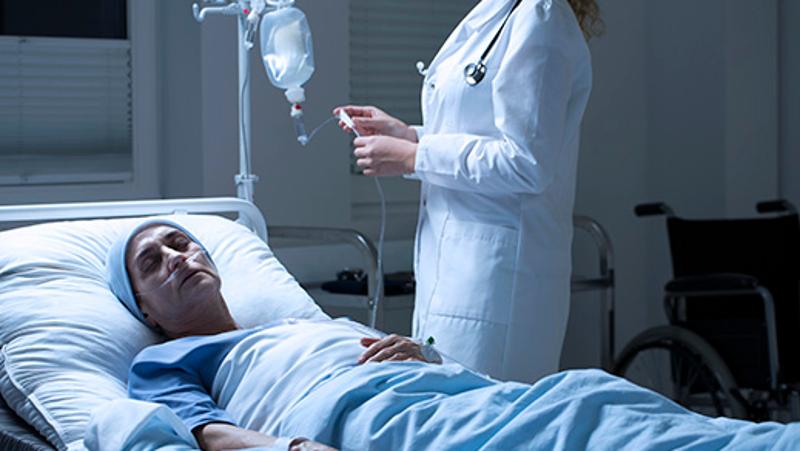
Some people receiving end of life care may not receive adequate pain and symptom relief when some clinicians who, unsure of the law, under-medicate due to concerns about legal liability.
- Some patients may be dying in pain because they are under-medicated due to fear of legal risk
- Australia's first online course for doctors on end of life law
- Free course aims to end significant knowledge gaps on end of life law in medical practitioners
- Significant legal reforms in end of life law over the past few years.
- Course covers end of life decision-making for children, advance care directives
- Withholding and withdrawing treatment, non-beneficial treatment and family conflict also covered.
A new free online course, End of Life Law for Clinicians, aims to improve knowledge in this area of law, to help doctors deal with these difficult treatment situations when they encounter them.
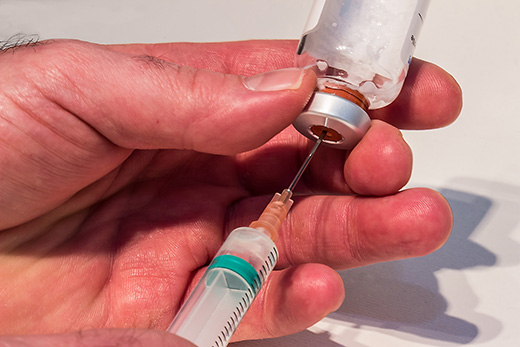
The course is the result of years of research by QUT Australian Centre for Health Law Research’s Professor Ben White and Professor Lindy Willmott on clinicians’ and the public’s knowledge of end of life law. It has been developed with QUT palliative care expert Professor Patsy Yates and health law researcher Dr Shih-Ning Then.
“Our previous research on withholding and withdrawing life-sustaining treatment from adults who lack decision-making capacity found significant knowledge gaps about end of life law among Australian medical practitioners,” Professor Willmott said.
“End of life care involves clinicians applying the law regularly: for example, when deciding whether to follow a person’s Advance Care Directive; how much morphine to administer to a dying patient; or whether life support should be withheld or withdrawn.
“Not knowing the law creates risks for clinicians including breaching the law, with the potential for civil liability or criminal prosecution, and this can lead to doctors practising defensive medicine and under-palliation of patients.
“It is an emotionally charged time and lack of knowledge about the law can lead to poor doctor-patient communication and conflict with patients’ and families.”

Professor White said legislators, the medical profession, and the broader community were grappling with significant legal changes involving complex ethical, moral and legal issues in end of life decision-making.
“We have seen significant legal reforms across Australia in the past few years that have implications for clinicians and the community, including reforms to Victoria’s medical treatment decision-making law,” Professor White said.
“High profile cases like Charlie Gard in the UK have also renewed debate about futile or non-beneficial treatment, and where we should draw the line when it comes to providing treatment to critically ill patients.”
The End of Life Law for Clinicians course has 10 30-minute online modules on capacity and consent to medical treatment, withholding and withdrawing treatment, Advance Care Directives, substitute decision-making, palliative medication, futile or non-beneficial treatment, emergency treatment, end-of-life decision-making for children, and managing disputes.
From early 2019, 22 training workshops across Australia will be delivered in addition to the online training. To view the workshop program visit End of Life Law in Australia or contact endoflifelaw@qut.edu.au.
QUT Media contact:
Niki Widdowson, 07 3138 2999 or n.widdowson@qut.edu.au
After hours: Rose Trapnell, 0407 585 901 or media@qut.edu.au.




